Purtscher's retinopathy
In this article we are going to address the topic of Purtscher's retinopathy, a topic that has been the subject of great interest and debate in recent years. Purtscher's retinopathy has raised mixed opinions and has been the subject of study by numerous experts in the field. Throughout this article we are going to analyze in depth the different aspects related to Purtscher's retinopathy, from its origin and evolution to its impact on current society. In addition, we will examine the different perspectives and approaches that exist around Purtscher's retinopathy, with the aim of providing a comprehensive and enriching vision on this topic. Without a doubt, Purtscher's retinopathy is a topical topic that deserves to be explored in detail, and we are sure that this article will provide a fresh and insightful perspective on the same.
| Purtscher's retinopathy | |
|---|---|
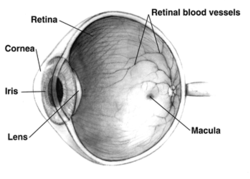 | |
| Anatomy of eye(Retina on top) | |
| Specialty | Ophthalmology |
Purtscher's retinopathy is a disease where part of the eye (retina) is damaged. Usually associated with severe head injuries, it may also occur with other types of trauma, such as long bone fractures, or with several non-traumatic systemic diseases. However, the exact cause of the disease is not well understood. There are no treatments specific for Purtscher's retinopathy, and the prognosis varies. The disease can threaten vision, sometimes causing temporary or permanent blindness.
It is named for the Austrian ophthalmologist, Othmar Purtscher (1852–1927), who detected it in 1910 and described it fully in 1912.
The term Purtscher-like retinopathy is used when there is no history of trauma.[1]
Presentation
Associated diseases
- Severe head, chest, or long bone trauma
- Acute pancreatitis
- Amniotic fluid embolism
- Chronic kidney failure
- Dermatomyositis
- Fat embolism syndrome
- Scleroderma
- Systemic lupus erythematosus (SLE)
- Thrombotic thrombocytopenic purpura (TTP)
Pathophysiology
Purtscher's retinopathy likely involves complex pathophysiology, with several contributing factors, including complement-mediated aggregates, fat, air, fibrin clots and platelet clumps.[2] The diseases leads to the formation of cotton wool spots in the retina, a finding observed in several other diseases, and atrophy of the optic nerve.[3]
Diagnosis
Where trauma is involved, only a funduscopic examination of the back of the eye (retina) is necessary to make the diagnosis.[3] Fluoroscein angiography may show a decrease in blood flow to the areas of whiteness in the retina. Typical features are Purtscher flecken (polygonal white areas in the retina) with perivascular clearing.
Treatment
It may be treated with triamcinolone in some cases.[4] However, in general, there are no treatments for Purtscher's retinopathy. If it is caused by a systemic disease or emboli, then those conditions should be treated.
Prognosis
Purtscher's retinopathy can lead to loss of vision,[5] and recovery of vision may occur very little.[3] However, vision recovery does occur in some cases, and reports have varied on the long-term prognosis.[6]
History
Purtscher's retinopathy was first characterized in 1910 and 1912 as a syndrome of sudden blindness after head trauma,[7] with patches of hemorrhage and whitening of the retina in both eyes.[3] Later, it was discovered to occur after other types of trauma, such as chest trauma, and is associated with several non-traumatic systemic diseases.[3] Purtscher's retinopathy may also be associated with acute pancreatitis, vasculitis, embolization of such materials as fat and amniotic fluid,[8] systemic lupus erythematosus, thrombotic thrombocytopenic purpura, and chronic kidney failure.[3] Purtscher's retinopathy may be caused by extensive fractures of the long bones.[9]
References
- ^ Tripathy K, Patel BC. Purtscher Retinopathy. 2023 Apr 3. In: . Treasure Island (FL): StatPearls Publishing; 2023 Jan–. PMID: 31194324.
- ^ Buckley, Sally A.; James, B (July 1996). "Purtscher's retinopathy". Postgraduate Medical Journal. 72 (849): 409–12. doi:10.1136/pgmj.72.849.409. PMC 2398519. PMID 8935600.
- ^ a b c d e f Yanoff, Myron; Duker, Jay S. (2008). Ophthalmology (3rd ed.). Edinburgh: Mosby. pp. 750–754. ISBN 978-0323057516.
- ^ Olson J, Rouhani B, Mandava N (March 2008). "Sub-Tenon's triamcinolone for post-partum Purtscher's-like retinopathy". Clinical Ophthalmology. 2 (1): 195–8. doi:10.2147/opth.s2080. PMC 2698687. PMID 19668404.
- ^ Agrawal A, McKibbin M (Nov 2007). "Purtscher's retinopathy: epidemiology, clinical features, and outcome". British Journal of Ophthalmology. 91 (11): 1456–9. doi:10.1136/bjo.2007.117408. PMC 2095457. PMID 17556428.
- ^ Schmidt, D; Otto, T (June 2004). "Prognosis and differential diagnosis of Purtscher's retinopathy". Der Ophthalmologe: Zeitschrift der Deutschen Ophthalmologischen Gesellschaft. 101 (6): 576–83. doi:10.1007/s00347-003-0952-6. PMID 15197574.
- ^ Purtscher O (1912). "Angiopathia retinae traumatica. Lymphorrhagien des Augengrundes". Albrecht von Graefe's Archiv für Ophthalmologie. 82 (2): 347–71. doi:10.1007/bf01929449. S2CID 40420476.
- ^ Retinopathy, Purtscher's at eMedicine
- ^ Chuang, EL; Miller FS, 3rd; Kalina, RE (March 1985). "Retinal lesions following long bone fractures". Ophthalmology. 92 (3): 370–4. doi:10.1016/s0161-6420(85)34023-x. PMID 3991127.
{{cite journal}}: CS1 maint: numeric names: authors list (link)